Get the latest Vera news
Stay current on healthcare industry developments, Vera updates, in-depth resources, and interviews with Vera providers and other industry experts. Sign up to receive our newsletter.
The fee-for-service system of healthcare won’t be sustainable for much longer. Payers who move quickly towards providing value-based care will gain an advantage over those who continue to operate a fee-for-service model.
Our new resource, Value-Based Care: What It Is, Why It’s Important, And The Best Way To Deliver It, takes a detailed look at the most important considerations for providers who are thinking about getting into the business of value-based primary care.
Payers need to control the total cost of care and deliver value. One of the most effective ways to do that is by taking an evolved approach to care delivery that builds on the foundation of population health management.
That approach is called advanced primary care, and it’s an effective tool for payers to close care gaps for at-risk population segments while controlling the total cost of care
Advanced primary care manages at-risk populations more effectively
The majority of healthcare costs are driven by the needs of a minority of patients. Population health management is built on a model that defines three segments of any given population.
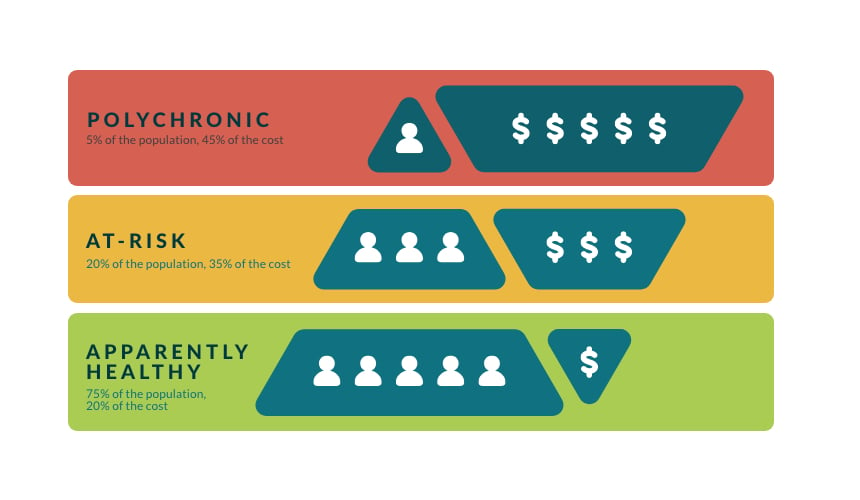
Only 5% of the population is polychronic (having multiple chronic conditions), but they typically account for 45% of the cost of healthcare.
Patients in this segment are dealing with serious health issues and have high-cost needs — ER visits, multiple extended hospital stays, and complex treatments.
This segment usually represents 20% of the population and accounts for 35% of the cost. They typically have underlying conditions and are at risk of becoming part of segment 1.
Rigorous primary care can have a major impact on this population by treating underlying conditions and empowering patients to make healthy lifestyle changes.
This segment is usually 75% of the total population but accounts for only 20% of the cost of care. This segment is defined by the fact that they have not yet generated a major health claim.
Effective population health management starts with understanding who is at risk. Although “at risk” and “not at risk” are common conceptions of segments 2 and 3,  the dividing line between these two groups is not clear-cut.
the dividing line between these two groups is not clear-cut.
In fact, there is no dichotomy between people who are “at risk” and “not at risk” for disease with regard to high blood pressure, cholesterol, alcohol and tobacco consumption, diet and weight, and other factors.
Disease risk is a continuum, and only a small percentage of any population is likely to be at either extremely high or low risk. The majority of people fall in the middle of the distribution of risk.
 This means we need to take a closer look at segment 3. They represent 75% of the population, and are often described as “generally healthy,” because they haven’t generated a major health claim. But appearances can be deceiving, and payers need to start thinking of this population segment in a different way.
This means we need to take a closer look at segment 3. They represent 75% of the population, and are often described as “generally healthy,” because they haven’t generated a major health claim. But appearances can be deceiving, and payers need to start thinking of this population segment in a different way.
In reality, people in segment 3 may not feel healthy at all. They may be in need of intervention to help them form healthier lifestyle habits. They may be at risk of developing chronic conditions.
Here’s the key point: most patients who are now in segment 1 were once part of segment 3. What can payers do to prevent that cycle from reoccurring?
The first step is to remove barriers that hold people back from seeking care:
The first barrier is prohibitive cost. If they are on a high-deductible health plan, they may have chosen not to pursue care because it’s too expensive.
The second barrier is lack of access or awareness. People in segment 3 may have never had the opportunity for an in-depth conversation with a health provider to uncover health risks and discuss their full bio, psycho, and social health. They may not know that they could benefit from more regular contact with a provider or from lifestyle changes.
Patients need a model of care that ensures they are fully engaged with their own health. They also need health appointments that give them enough time to connect with a primary care provider who can help them identify hidden risks.
Our new resource, Value-Based Care: What It Is, Why It’s Important, And The Best Way To Deliver It, details how value-based care is more effective at reducing total cost and managing population health. An advanced primary care model allows payers to reduce the total cost of care by identifying invisible risk early (regardless of whether a patient has filed a major claim) and then helping at-risk patients become truly healthy instead of developing more complex and costly conditions.
Stay current on healthcare industry developments, Vera updates, in-depth resources, and interviews with Vera providers
Stay current on healthcare industry developments, Vera updates, in-depth resources, and interviews with Vera providers and other industry experts. Sign up to receive our newsletter.