It isn’t always easy to help your patients achieve healthy behavior change. But the events of 2020 showed that even in difficult circumstances, behavior change is possible for your patients — and it’s an integral part of effective primary care that leads to better health outcomes.
The widespread adoption of telehealth during the COVID-19 pandemic is a huge opportunity to promote behavior change — giving patients more opportunities to connect with healthcare professionals face-to-face and get necessary support. But although 2020 made this opportunity clear, we know that new technology isn’t enough on its own.
The key to lasting behavior change is to make sure providers and health coaches have the time and resources they need to truly connect with each patient, help them identify health goals, and support them every step of the way.

Behavior change transforms health outcomes
There are few experiences more rewarding than helping a patient adopt habits that have a positive effect on their future health. 2020 demonstrated the incredible importance of even the simplest behavior changes, like wearing a mask and remembering to stay six feet apart.
Dive Deeper: Behavior Change: The Path Towards Health Transformation
But as you know, behavior change is often “easier said than done.” Many primary care providers aren’t able to focus on prevention and lifestyle changes as much as they’d like to.
And without the time and resources to make behavior change possible, the only option is to refer the patient to a specialist and hope for the best. It can be frustrating to only have the ability to address a patient’s immediate symptoms — especially when there is so much potential for more lasting change

If primary care created space to focus on behavior change, it could dramatically reduce the number of chronic (often preventable) conditions that currently affect 6 in 10 US adults. Behavior change must start in the primary care setting. Why? Because behavior change doesn’t happen in a moment.
Some behavior changes take months or years of effort — like smoking cessation, transitioning to a healthier diet, or living a more active lifestyle. Patients need long-term support from a trusted provider to make these changes. That’s why primary care is the ideal setting to invest in behavior change and why Vera makes it a priority.
Breaking down barriers to behavior change
Even when patients and providers both know the potential positive impact, behavior change can be incredibly difficult to achieve. Even without the added pressure of COVID-19, providers working in a fee-for-service model are rarely able to take the time they need to connect with each patient and guide them towards behavior change.
You may be working in an environment where the pressure of back-to-back appointments only lets you treat immediate symptoms and refer patients to specialists. That’s why Vera’s model of advanced primary care is based on value, not volume. Our goal is to give providers the time and resources necessary to build trust with each patient, learn their individual story, and address root causes of health issues. For our providers, helping patients achieve healthy behavior change isn’t just a goal — it’s a reality.

But during a year of disrupted routines and remote communication, were providers still able to forge meaningful connections with patients and promote healthy changes?
Telehealth and virtual care: A promising way to engage
As you know, the COVID-19 pandemic caused a dramatic acceleration in the use of telehealth. Despite the challenges of moving to remote care so quickly, both patients and providers report a positive response to this newly essential mode of care delivery. In other words, the convenience of telehealth has meant even more opportunities to connect with patients and guide them towards positive behavior change.
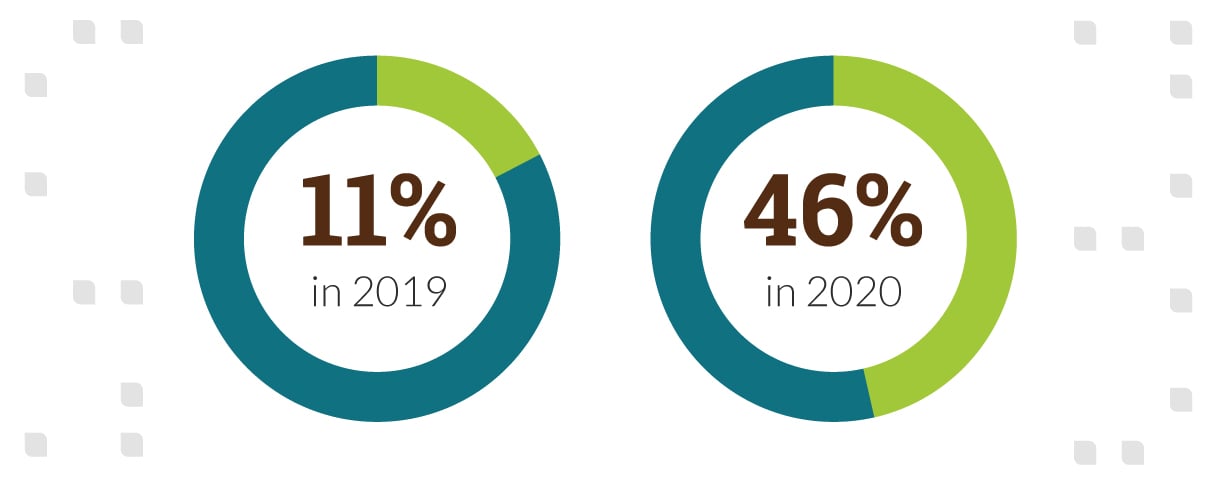
Consumer adoption of telehealth has skyrocketed:
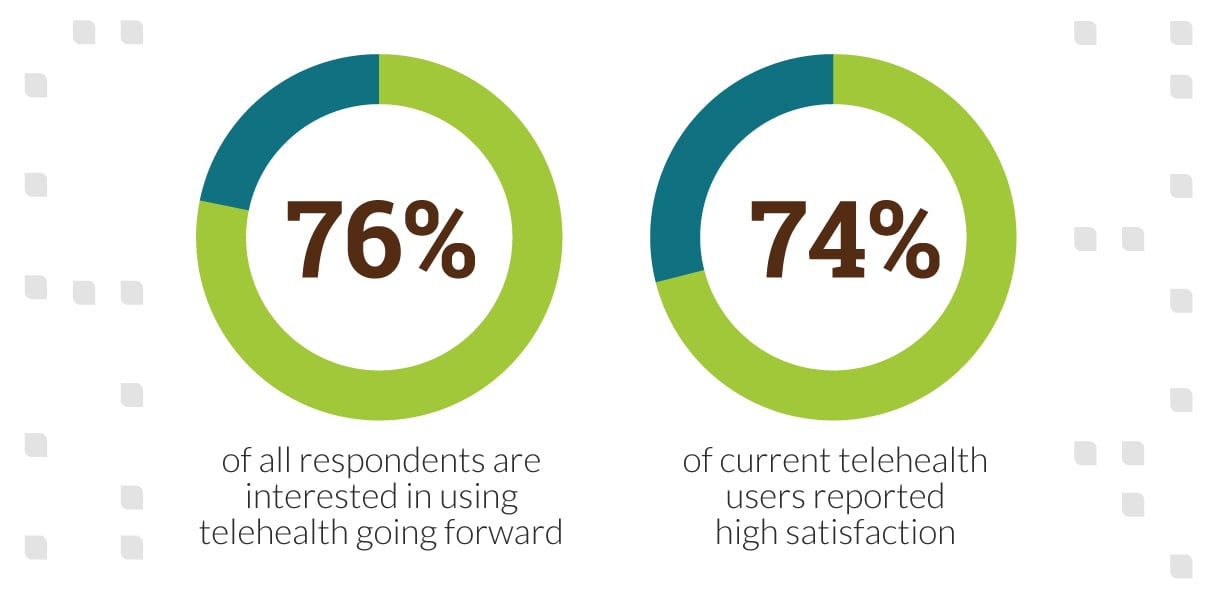
Patients see telehealth as a good thing:
- 76% of all respondents are interested in using telehealth going forward
- 74% of current telehealth users reported high satisfaction (McKinsey)
The regulatory outlook for telehealth is positive:
- CMS temporarily approved 80 new telehealth services and added regulatory flexibilities to increase access to virtual care (McKinsey)
Telehealth is an opportunity to expand access to essential care, particularly those who are underserved. When a virtual care option is easy to navigate, it can also reduce “no show” rates and help patients stay engaged with treatment plans and make progress on long-term health goals. At Vera, we make sure providers don’t need to rush appointments — whether they take place in person or remotely.
“Right now, we’re also doing a lot of our wellness visits via video. And we’re able to spend that good 30 to 45 minutes with the patient, really connecting, talking about either their chronic diseases or just what’s going on with them at that time.” — Sue Ferbet, Vera Whole Health Chief Clinical Operations Officer
During COVID-19, many people are dealing with symptoms of depression, anxiety, and adjustment disorder — difficulty handling numerous fast-paced changes. Virtual care can also be a helpful tool in connecting patients with behavioral health care and health coaching.
“This is a prime time for coaching, if people take advantage of it — you have somebody that listens to you with no judgment. You have that space to talk through things, somebody to help you plan. I think people are ready for that now.” — Cheridan Bryant, Vera Whole Health Coach Operations Manager
2020 proved that even in the most difficult circumstances, it’s still possible to support patients with true behavior change that transforms the course of their health and future. How? By increasing access to care, building a personal connection based on trust, and providing each patient with effective health coaching.
Discover how you can spend more time listening to patients and treating their whole health with our unique model of advanced primary care.
Or, learn more about the science of behavior change and how you can use it to help patients improve their health by checking out our FREE guide, Behavior Change: The Path Towards Health Transformation.
Sign up
Join our email list to receive the latest open positions, Vera Careers news, and more.