As healthcare costs rise, organizations struggle to provide the benefits members need and the care services they want. Results from our new survey reveal that even well intentioned benefit strategies can end up restricting organizations due to lack of control, rising costs, and meager services.
The pain of rising costs and insufficient member benefits underscore the need for a more holistic healthcare solution that reduces overall costs. We hope the survey results and takeaways below help your organization balance the cost of healthcare with proven outcomes for members.

A high-level look at the results
Our third-party survey gathered responses from 114 qualified professionals. The two largest groups of respondents had either been with their current organization for one to three years (32%) or 11+ years (30%). Respondents were asked questions about their current state of benefits and upcoming plans across the industry. Many results reveal healthcare’s strain on organizations and members.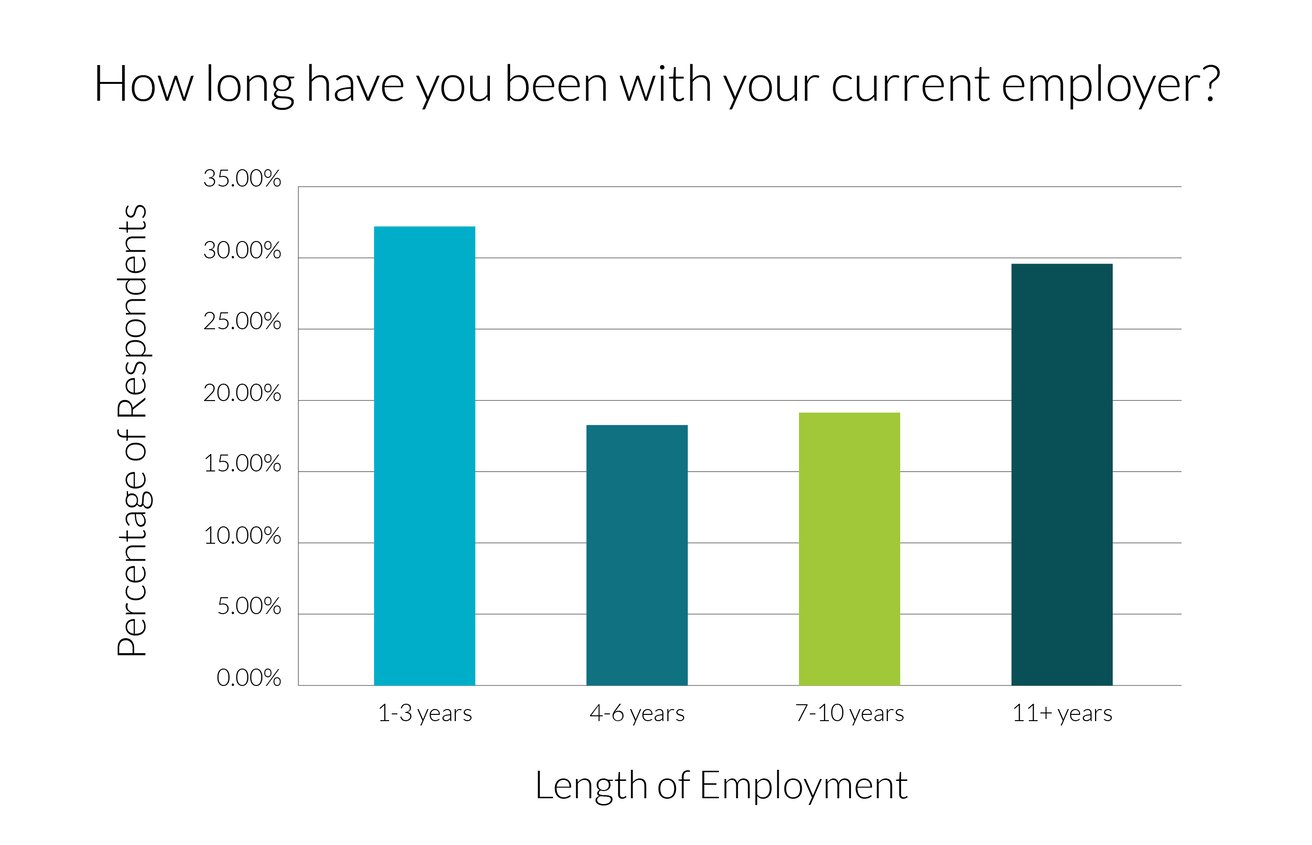
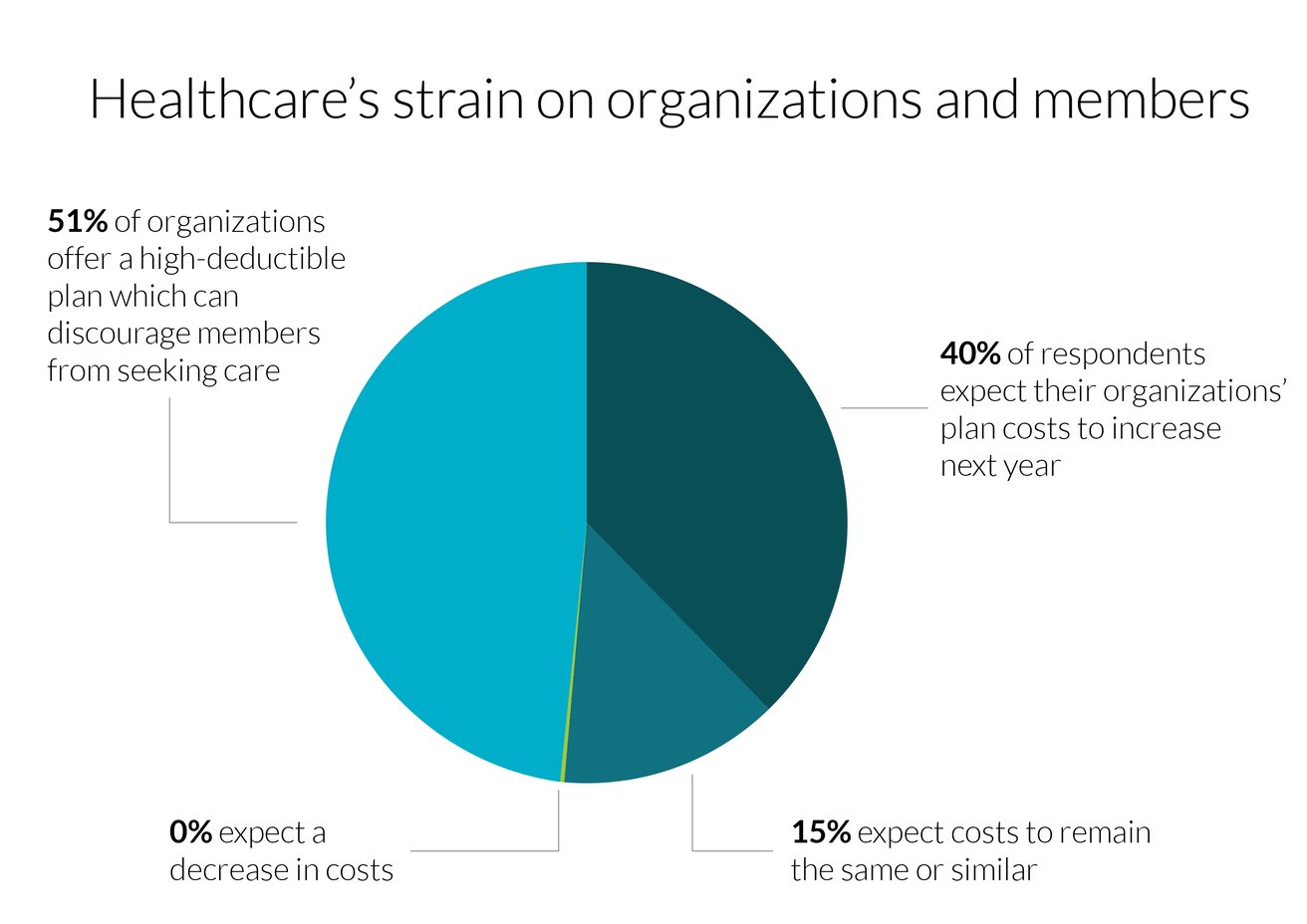
When asked which areas of their current benefit plan they wish were better, respondents wanted to see:
- Lower premiums and other cost reductions for the organization and their members
- More affordable dental coverage
- More expansive provider selection and better overall coverage, including:
- reproductive care
- preventive care
- massage therapy
- vision
To be clear: The problem is not benefit managers' level of experience. Respondents with short and long tenures are feeling the strain of traditional benefit packages on their organization's budgets and members.
Results on rising costs
It’s understandable that part of maintaining organizational health is proactively identifying and quantifying important expenditures as a percentage of the overall budget. Few buckets are more consequential than benefits. Our survey revealed:
- Over 30% of respondents’ organizations cover 50% of members’ premiums
- 36% of respondents’ organizations cover 25% of members’ premiums
- These members pay an average of 28% of earnings for their contribution costs
- 72% of respondents said the financial responsibility placed on members’ shoulders was reasonable given what other organizations offer.
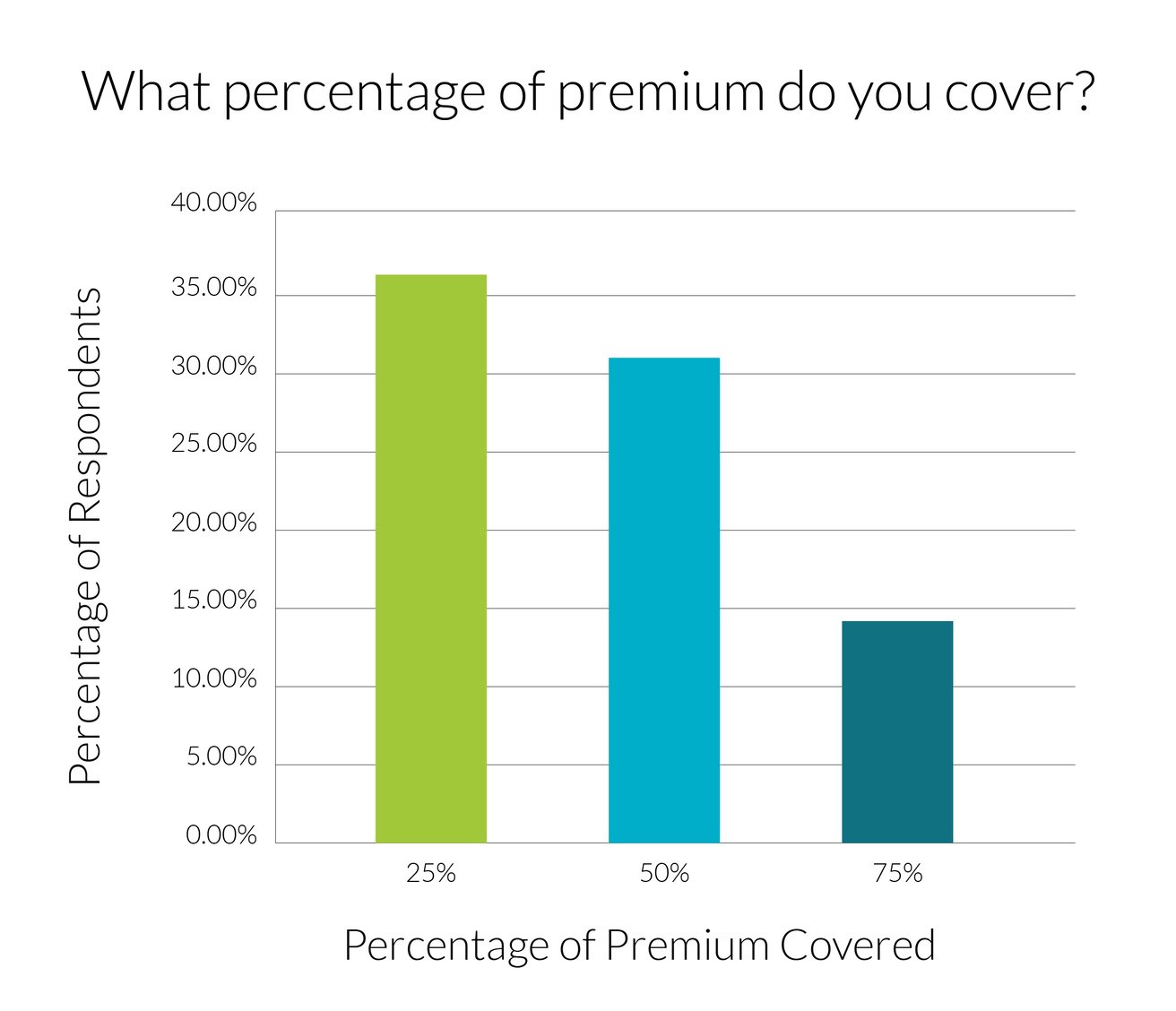
The table above shows the three prevailing answers from 80 percent of all respondents. As you can see, the data indicates that rising costs burden organizations and get passed along to their members — and often without a robust suite of benefits to justify the increasing expense.
Results on holistic benefits
While benefit managers are aware and supportive of employees' multifaceted needs, they often struggle to provide richer benefit packages due to rising costs. As a result, employees must look outside their workplace benefits to meet their needs:
- Only 64% of respondents’ organizations offer an employee assistance program or counseling
- Only 52% of organizations offer a wellness program, and just 20% of those same organizations include an incentive for members who participate in the wellness program
- A mere 11.5% of respondents’ organizations offer a gym membership
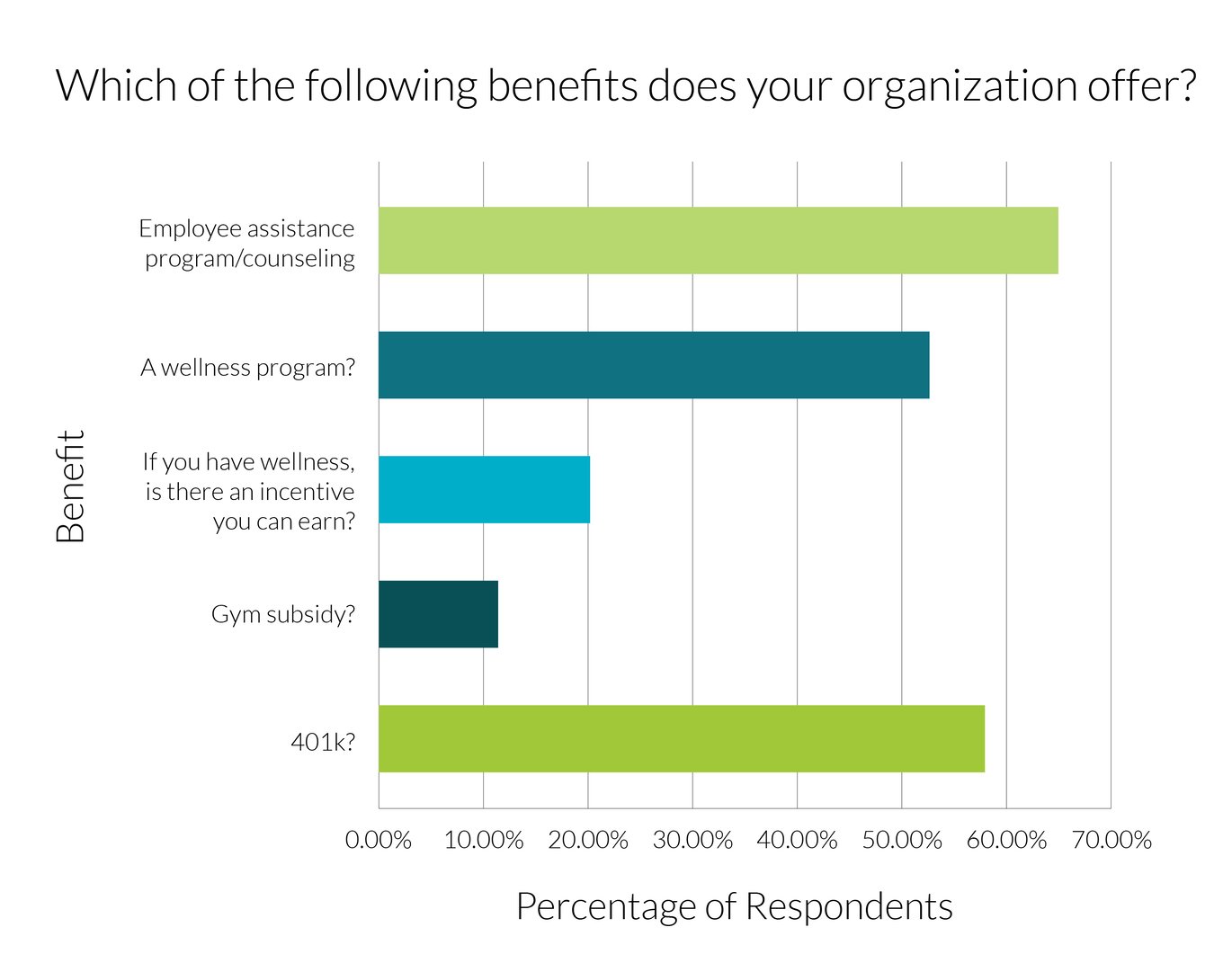
There's a solution in sight: Investing in healthcare that supports the bio-psycho-social needs of members (and is proven to increase health outcomes) will reduce absenteeism, improve happiness and healthcare quality scores, and increase acquisition and retention.
Results on the healthcare renewal process
The vast majority of respondents’ organizations evaluate their benefits and programs annually. With innovation reaching new heights all the time, the renewal process presents a great opportunity to collaborate with vendors who can help clarify the benefit process and work with organizations to design care models that align with their needs (rather than vendor’s needs).
Read our post: Common Sticking Points When Designing An APC Solution With A Vendor
At the end of the day, organizations should be able to count on the healthcare renewal process as a time where they can take meaningful steps towards getting related spending under control while delivering benefits that truly matter to members.
The pain of the status quo
We identify two immediate takeaways from the survey’s results:
- Organizations have grown accustomed to the broken traditional fee-for-service healthcare model with its skyrocketing annual renewal increases and high out-of-pocket costs for members (like premiums, copays, and deductibles).
- Organizations feel reassured about offering benefit packages similar to prevailing trends — even if the trends paint an unsustainable picture for organizations and members alike.
Traditional healthcare is still creating far too many pain points for organizations and members. At the same time, many organizations are taking a fresh look at their benefit strategies and are moving towards benefits that offer far more holistic solutions.
The answers can be found in an advanced primary care (APC) model that reduces overall healthcare costs and improves health outcomes with proven services including low- or no-cost primary care for members.
APC streamlines care and costs
Prohibitive cost burdens and underwhelming health outcomes will inevitably make organizations less competitive over time. We believe healthcare should deliver on its promises of improved health for the whole person while returning control to organizations and significantly reducing overall healthcare spending.
By making a financial allocation in APC, organizations drive member utilization through primary care which can provide 90 percent of all health-related care. APC reduces uncontained downstream care across all other portions of the healthcare system; the result is a significant return on investment through a reduction in total cost of care — and improved health outcomes resulting in happier, healthier members.
Want to learn more about a revolutionary win-win that’s reducing overall healthcare costs while driving real-world results? Read about the numerous benefits advanced primary care offers organizations and members in our new APC guide.